Recently, the number of people suffering from pancreatitis has been increasing. Doctors and nutritionists assure that in order to improve health, one should definitely adjust the diet. The question arises, what kind of diet for pancreatitis contributes to recovery? How to eat properly with this disease? Are there foods that can make the condition worse? What should you eat to improve your health?
Basic nutrition rules for pancreatitis
Diet is mandatory for those suffering from pancreatitis, otherwise no medicine will help.

Experts have developed rules that must be followed:
- if the disease is acute, then the diet should be started with fasting, lasting from 2 to 4 days;
- you must eat often, at the same time;
- portions should be small;
- avoid overeating;
- reduce the amount of confectionery products;
- meals should contain pureed products that do not irritate the mucous membrane;
- the daily norm of fat does not exceed 80 g;
- reduce the amount of salt to 10 g;
- keep sugar intake to a minimum.
Based on these rules, the daily menu is formed.
How to eat with acute pancreatitis
Acute pancreatitis is a dangerous disease, so comprehensive measures are needed to improve the condition. It must be remembered that dietary requirements are mandatory, otherwise this condition may lead to surgical intervention.
In the first phase of treatment, you should fast for several days. The duration of food refusal is from 2 to 4 days.
Only liquids are allowed. At this time, you can drink not strong tea, prepare rosehip decoctions, mineral water is suitable without gas.
The next step is diet number 5. Food has a low calorie content, salt and fat are prohibited, which can cause a new attack. All dishes are cooked in liquid form. You can add a lot.
It is best to keep a list of useful and harmful products at the beginning of the chapter when compiling the menu.
If you do not follow strict dietary rules, then the patient's condition will not improve.
How to eat with chronic pancreatitis
Nutrition in this disease should help normalize the work of the diseased organ. You should follow the advice of child no. 5.
Diet tips for chronic pancreatitis:
- food and liquids entering the body should be warm;
- plan at least 5 meals during the day;
- avoid overeating;
- do not take long breaks between meals;
- reduce the amount of sugar;
- take out the fresh bread.
All dishes prepared by frying are strictly prohibited.

To form a proper diet, you should know the list of products that will help you recover or worsen your health.
Table of permitted and prohibited products:
- bakery products: crackers, dried yesterday's bread, biscuits;
- porridge cooked in water with a little milk;
- meat, steamed, in the oven, boiled chicken, turkey, lean beef;
- low-fat fish, pureed, chopped;
- first courses: lean, vegetable, pureed soups;
- dairy products: all of them should be non-acidic, they can be low-fat;
- vegetables: no coarse fibers;
- non-sour fruit;
- no more than 1 egg per day;
- butter no more than 30 g per day;
- vegetable oil no more than 2 tablespoons;
- non-acidic juices diluted with water;
- the tea is not strong, it can be with lemon, milk;
- bakery products: fresh bread, muffins, puff pastry products;
- soups cooked in strong broth;
- fatty meat;
- high-fat dairy products;
- sauces;
- spices;
- fatty fish;
- fried eggs;
- vegetables with coarse fibers;
- mushrooms;
- legumes;
- carbonated beverages;
- alcohol;
- coffee;
- chocolate.
If you have questions, it is recommended that you discuss the use of certain products with your doctor.
Diet for pancreatitis in children
Parents often have a question, what kind of diet for pancreatitis does a sick child need? The diet, which helps to improve the condition of the baby, is slightly different from the menu of adults. But there are some peculiarities that should be taken into account when feeding children.
Children's nutrition rules:
- give food and drink warm, feed more chopped food, for example, mashed potatoes;
- nutrition should contain all components necessary for normal growth and development;
- even after removing the acute condition, it is necessary to adhere to dietary restrictions;
- forbid children to drink carbonated drinks;
- fast food dishes.
If the sick child is not even 3 years old, then it is recommended to wipe the food, grind it. All citrus fruits and freshly squeezed juices should be excluded from the diet. Children should not be given berries with small seeds and rough skin. Fresh vegetables are not required.

A child over the age of 3 attends children's educational institutions, contacts with peers. First of all, you have to take care of nutrition in school and kindergarten. To do this, talk to the medical worker, inform the teacher, the educator.
The most difficult thing is to protect the child from soda, chips and other dangerous foods. When going to birthday parties and children's parties, you should make sure that the child does not violate the diet. The child should explain the need to limit food.
Menu for 7 days for patients with chronic pancreatitis
Patients are recommended to prepare a menu in advance, which will allow you to eat a balanced diet, while the state of health will noticeably improve.
Menu option for the week:
1 day
- chicken meat, rosehip soup;
- oatmeal, tea;
- pumpkin soup, steamed fish, jelly;
- Baby food jar;
- stewed zucchini, carrots, chicken fillet from the oven, juice;
2 day
- rice porridge, tea with honey;
- pumpkin puree, compote;
- puree for vegetable soup, chicken meatballs, jelly;
- tea, crackers;
- semolina pudding and jelly;
3 days
- oatmeal, jelly;
- baked apple with cottage cheese, rosehip soup;
- vegetable puree soup, steamed fish, compote;
- fresh cheese, tea;
- boiled fish, tea;
Day 4
- rice porridge, crackers, rosehip soup;
- pumpkin puree, tea;
- vegetable soup, a piece of boiled fish, mashed potatoes, compote;
- tea with honey, biscuits;
- rice pudding, jelly;
5th day
- oatmeal, tea;
- fresh cheese, baked apple, rosehip soup;
- vegetable soup, chicken meatballs, compote;
- tea, dry biscuits;
- fish baked in the oven, rosehip soup.
6th day
- semolina, tea;
- baked apple, rosehip soup;
- vegetable soup with a piece of beef, vegetable puree, compote;
- tea, crackers;
- steamed omelette, jelly;
7th day
- rice porridge, crackers, rosehip soup;
- fresh cheese with chopped apple, tea;
- puree for vegetable soup, chicken meatballs, jelly;
- cottage cheese, tea, biscuits;
- semolina pudding, jelly.
Knowing the basic requirements for dishes, you can create your own menu.
Recipes for pancreatitis

Knowing the basic rules of nutrition, you can make changes in the menu. With food restrictions, you want to settle for something delicious. Nutritionists have developed special dishes that can be consumed with pancreatitis.
Recipe for baked apples:
- Remove the core from the washed apples, being careful not to pierce the bottom of the fruit.
- Put the honey in the apple.
- Add cinnamon on top.
- Bake in the oven.
- Take it easy.
Recipe for beetroot salad:
- Boil 1 medium-sized beet, cool, grate.
- 2 sweet apples, peeled, cut into small cubes.
- Grind the walnuts on a grater, you need about a spoon.
- Combine all components, mix, add a little salt.
- Fill with olive oil.

Recipe for semolina pudding with berry jelly:
- Prepare a thick semolina porridge in water, pour it into deep moulds, let it cool.
- Cover the strawberries with a little water, boil, remove, chop, return to the broth.
- Pour sugar, heat to boil.
- Prepare the starch, mix in cold water, carefully pour into the strawberry soup, bring to a boil, without letting it boil. Remove from heat, cool.
- When serving, cut the thickened semolina pudding into pieces, pour jelly on top.
If desired, each diet can be supplemented with delicious healthy dishes.
We recommend a video on permitted and prohibited foods for pancreatitis:
Pancreatitis is a common disease that requires a strict diet for treatment. To do this, you need to know which foods can and cannot be consumed. Cooking rules, general dietary recommendations should be followed.
Types of pancreatitis
The most general classification of pancreatitis is based on the nature of the course of the disease: acute attack or long-term chronic pancreatitis with periodic relapses. These two forms differ in the severity of symptoms and require different approaches to treatment.
Acute pancreatitis
The inflammatory process in acute pancreatitis develops very quickly and is always accompanied by severe pain. In most cases, the disease occurs against the background of alcohol abuse or after consuming a large amount of fatty food. Sometimes the exacerbation is preceded by an attack of acute hepatic colic.
Symptoms of acute pancreatitis:
- Severe pain in the left hypochondrium that spreads to other organs. The pain attack lasts about half an hour to an hour. The pain is especially strong when you lie on your back. The attack worsens after eating, especially fried and spicy food, and any alcoholic beverages.
- Vomiting, often violent, bilious and bitter. Constant nausea that does not go away after vomiting.
- Subfebrile or high fever.
- Sometimes, due to a violation of the outflow of bile, the yellowness of the eye proteins is observed, very rarely - a yellow shade of the skin.
- In some cases, the pain syndrome is accompanied by heartburn and bloating.
An attack of acute pancreatitis requires immediate medical attention. Painkillers bring only temporary relief, but do not affect the cause of inflammation. In the absence of qualified help, the risk of serious complications increases rapidly: infections of inflamed tissues, necrosis and abscesses.
Acute pancreatitis in a severe stage can lead to shock and multi-organ failure.
Chronic pancreatitis
If after an attack of acute pancreatitis a person does not follow the doctor's recommendations and continues to drink alcohol and eat unhealthy food, there is a high probability that the disease will become chronic. Chronic pancreatitis develops with significant damage to the pancreas during the first episode of the disease.
The disease is characterized by gradual pathological changes in the structure of pancreatic cells. Over time, it begins to lose its main function - the production of enzymes necessary for food digestion. Exocrine insufficiency is manifested by:
- diarrhea
- flatulence,
- change in the nature of feces - they acquire a sticky consistency due to the large amount of fat in them and are poorly washed off the walls of the toilet bowl.
Chronic pancreatitis can be asymptomatic for a long time: acute pain occurs when significant pathological changes have already occurred in the pancreas. During an attack, chronic pancreatitis manifests itself with the same symptoms as acute:
- severe pain in the waist,
- nausea,
- throw up
- intestinal disorders.
The diagnosis is made on the basis of ultrasound, computer tomography or magnetic resonance. During the study, narrowed ducts of the pancreas are usually found due to the formation of stones in them - calcification. Hardware techniques also allow the detection of cysts at the site of atrophied tissue. Laboratory blood tests for chronic pancreatitis are not very informative.
Pancreatic insufficiency is determined by faeces analysis. If they contain a specific enzyme - pancreatic elastase - the diagnosis "chronic pancreatitis" is made.
Importance of enzymes in digestion
The functioning of the human body provides a complex system of interconnected and interdependent biochemical reactions. Thanks to special protein compounds - enzymes or enzymes - all these reactions are accelerated, ensuring fast metabolism. The action of enzymes is very selective: each of them can initiate, accelerate or slow down only one reaction.
Digestion is based on the work of digestive enzymes. Their main task is to make the energy assimilation process fast and efficient. Enzymes break down food components (proteins, fats and carbohydrates) into absorbable substances. At the same time, the amount of enzymes produced depends on the quantity and quality of food.
Food digestion begins in the mouth. Food crushed by the teeth into small pieces is mixed with saliva, which contains the enzyme alpha-amylase. The better we chew our food, the easier it is for the salivary gland enzyme to convert starch molecules into soluble sugars and facilitate further processing.
After initial processing, food enters the stomach through the esophagus, where the gastric enzyme pepsin and hydrochloric acid begin to act. These substances create gastric juice, which:
- provides antibacterial protection of the body;
- stimulates the production of pancreatic hormones;
- regulates the motility of the stomach;
- breaks down fats and performs a number of other functions.
In addition to pepsin, which is responsible for breaking down large protein molecules, other enzymes are also produced in the stomach, for example:
- gelatinase - a solvent for collagen, gelatin and other connective tissue proteins;
- lipase - an enzyme that breaks down certain fat molecules into fatty acids and monoglycerides;
- chymosin - starts the process of digesting milk proteins.
Bile plays an important role in the digestion process. It contains bile acids that stimulate the production of pancreatic secretions.
From the stomach, the bolus of food is evacuated into the duodenum, where the main process of food digestion takes place. It is provided by more than 20 pancreatic enzymes. Enzymes are found in pancreatic juice, which is produced by the gland in the amount of about two liters per day.
Functions of pancreatic enzymes:
- proteases - breakdown of proteins into amino acids;
- nucleases - act on nucleic acid DNA;
- amylase - breaks down starch into simple sugars;
- lipases - break down fats into more fatty acids and glycerol.
Due to the violation of the function of enzyme production by the organs of the digestive system, especially the pancreas, the whole organism is unbalanced. This imbalance leads to nausea, diarrhea, bloating, followed by anemia and malnutrition.
What to take with food with pancreatic enzyme deficiency
In pancreatitis, the process of production of digestive enzymes of the pancreas is disturbed, due to which the person suffers from discomfort and pain in the stomach. In that case, after a complete examination, substitution therapy can be prescribed.
The task of treatment with enzyme preparations is to compensate for their deficiency in the body, while reducing the load on the damaged organ. In some cases, such therapy is prescribed for life.
Important!The action of all enzyme preparations begins 20-30 minutes after a meal, so you must drink them strictly before eating in the dose prescribed by your doctor!
Modern pharmacology offers a large number of different enzyme preparations of animal and plant origin. Some of them are aimed only at filling the deficiency of one enzyme, for example, the breakdown of lactose or fat. There are also means of complex action, prescribed for the lack of several enzymes in various organs of the digestive system.
Pancreatic enzymes are obtained from the organs of cows or pigs. The composition of the drugs includes the main pancreatic enzymes - amylase, lipase and trypsin. In addition to pure pancreatin, polyenzyme preparations may include bile acids, adsorbents or other enzymes. All drugs are selected strictly individually, taking into account the nature of the course of the disease and the severity of the symptoms.
What is the diet for pancreatitis?
In the process of treating pancreatitis, nutrition plays no less role than drugs. The main goal of the prescribed diet is to restore the functions of the pancreas and normalize the production of digestive enzymes.
Food that is difficult to process increases the load on the inflamed organ. After an abundant feast with fatty fried food, the pancreas begins intensively producing enzymes for its digestion. If the ducts of the gland are narrowed, pancreatic juice produced in extreme mode accumulates in the gland, worsening the development of the disease - the affected pancreas begins to digest itself.
Signs that your gland is going into overdrive include:
- heaviness in the stomach after eating,
- heartburn,
- burping
- attacks of stomach pain.
Of course, constantly following a strict diet is not easy, especially at home. People with severe dietary restrictions are forced to cook for themselves and resist the temptation to eat anything fried or spicy.
It is important to understand that one violation of the diet can cause an acute attack of pancreatitis with all the resulting consequences: severe pain, nausea, vomiting and diarrhea. One failure can undo all efforts to maintain long-term remission.
Diet rules number 5: what you can and can't eat with pancreatitis
Diet for pancreatitis has many restrictions on both the allowed food and the way it is prepared. Especially for people who have problems with the pancreas, one of the founders of domestic dietetics and gastroenterology, Professor I. I. Pevzner developed diet table number 5.
But, before getting acquainted with the special provisions of this diet, it is necessary to take into account the general principles of nutrition for pancreatitis:
- you must eat 5 times a day in small portions;
- exclude fried and sour foods;
- in the acute phase of the disease, food must be crushed or wiped;
- animal proteins should predominate in the diet;
- the daily amount of fat must not exceed 50 g;
- sugar is also strictly limited - no more than 30 g per day;
- products that increase flatulence are prohibited - sweet carbonated drinks, any legumes, sweet apples and grapes, sweet muffins and some others;
- salt intake is minimized - no more than three to five grams.
Important!With pancreatitis, you can eat slow carbohydrates, while you must monitor the ratio of nutrients in meals. Don't be fooled by the fact that sugar can be replaced with honey, its consumption should also be controlled. In the beginning, you will definitely need a calculator. It is necessary to immediately calculate the daily calorie intake and the balance of proteins, fats and carbohydrates based on the body mass index. This information is easy to find on the Internet on sites dedicated to proper nutrition and a healthy lifestyle. There are various mobile apps for counting calories and nutrients.
All these principles are taken into account in diet number 5, which exists in a basic and advanced version.
The basic option is indicated for relapses of chronic pancreatitis and for the acute nature of the disease. In the acute phase, the diet is stricter with numerous restrictions. It is aimed at relieving the pancreas and alleviating the symptoms of acute inflammation. In the first 3 days of the acute stage, the patient is recommended to starve in order to rest the pancreas. Furthermore, within 3-7 days, carbohydrate foods are allowed in small portions at short intervals. The caloric content of the diet these days should be reduced, and food should be consumed only in pureed or semi-liquid form.
Important!It is widely believed that rich soup, especially chicken soup, helps well with all digestive problems. Fatty soups are categorically contraindicated in pancreatitis, gall bladder disease and other pathologies of the gastrointestinal tract! An excessive amount of animal fat significantly increases the load on the pancreas and prevents the normalization of the condition.
The diet includes cereals on water and vegetable soups with various grains, except for millet and corn, boiled or steamed pureed vegetables. As for drinks, weak tea, jelly, dried fruit compote are allowed. Bread is allowed only white and slightly dried, you can eat crackers and biscuits like biscuits.
On the third day of the carbohydrate diet, protein products are gradually introduced:
- soup from lean meat, it is preferable to cook soup from veal, turkey or chicken breast, the meat from the soup should be passed through a meat grinder or chopped in a blender;
- steamed omelette or soft-boiled eggs;
- steam cutlets from lean meat or low-fat fish;
- cottage cheese casseroles and cottage cheese souffles with minimal fat content.
Diet number 5 is recognized as sparing the pancreas as much as possible, which in the acute phase needs complete rest. Allowed and prohibited foods for basic nutrition are shown in table 1.
Important!Predominance of protein foods in the diet can lead to constipation. In that case, you have to add more raw vegetables and fruits from the list of permitted ones. With gout, preference is given to proteins of vegetable origin or sea fish.
Can chronic pancreatitis be cured?
So far, no drug has been developed that would stop and reverse the processes that occur in the pancreas during chronic inflammation. Therefore, treatment is aimed at slowing down the progression of the disease and preventing it from worsening. In later stages, when there is a significant decrease in pancreatic function, therapy is supplemented with means to normalize digestion and blood sugar levels. Proton pump inhibitors, antispasmodics, painkillers, enzyme preparations are used to achieve remission of chronic pancreatitis, their choice is individual and depends on the clinical picture of the disease.
An important area of prevention is the timely treatment of diseases that lead to the development of chronic pancreatitis.
How to eat with chronic pancreatitis?
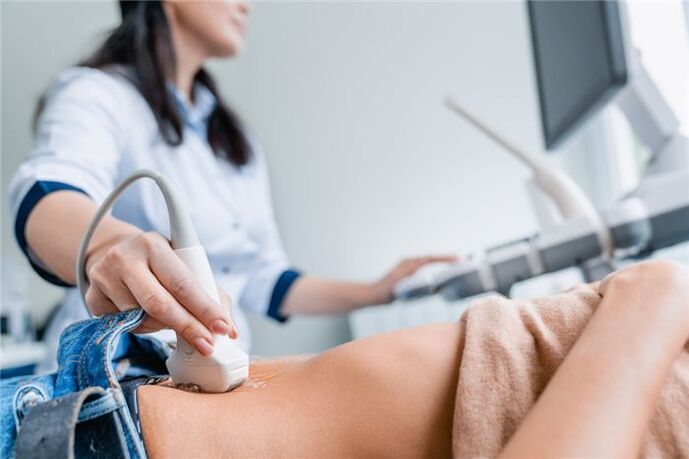
Compliance with a therapeutic diet is an effective, scientifically proven remedy for the prevention of inflammation. There are several modifications of therapeutic diets for the stage of exacerbation and remission. The diet used is based on the exclusion of products that stimulate an increase in gastric and pancreatic secretion. Resting the pancreas is very important to reduce inflammatory activity. In the acute phase, the deleted version of the diet is used, and when it goes into remission, the version without puree is used.
With chronic pancreatitis, it is important to provide the body with a sufficient amount of protein, the diet includes 110-120 g of protein per day, which slightly exceeds the physiological norm. At the same time, 60% of this amount should be animal proteins. The menu includes dishes from lean meat, poultry, fish, fresh cheese and egg whites. But fats and simple carbohydrates, on the contrary, are limiting.
Nutrition in chronic pancreatitis should be regular and fractional - 5-6 times a day in small portions. More about nutrition for pancreatitis































